What Causes Bunions & What You Can Do About Them
More than 40% of older adults develop bunions in their lifetime. In this article, pedorthists at Kintec share what causes bunions, and what to do about it. Let’s start by answering the most important question: what is a bunion?
What is a bunion?
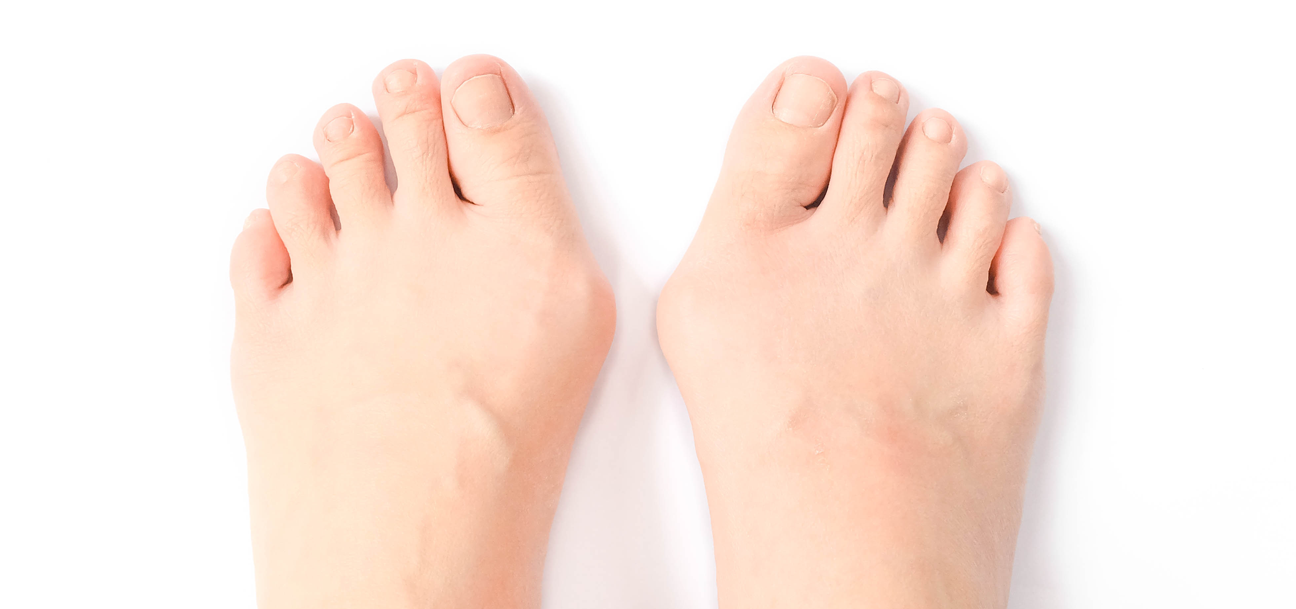
A bunion is a common, progressive bony disorder. It results in a bump on the side of the main joint of your big toe. However, a bunion is more than just a bump; it’s a result of significant changes to the bony architecture of the foot.
These changes start with the big toe – or hallux – moving toward the other toes. This makes it appear crooked, which is called hallux valgus. This movement can progress over time, resulting in a larger bump and painful symptoms such as inflammation and stiffness in the joint.
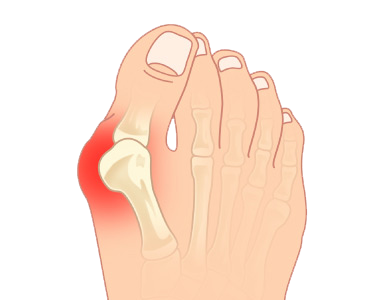
Symptoms of Bunions
Symptoms usually become noticeable later in the development of the bunion. However, some people never experience symptoms. Bunion symptoms may include:
- Skin irritation or redness over the bump
- Pain in the big toe joint – also known as the first metatarsophalangeal joint
- Swelling, limited mobility, or a burning sensation around the first MTP joint
- Callusing under the affected toe, on the side or under the joint next to it (second MTP joint)
- Difficulty with footwear fitting
- Pain in certain types of footwear and when walking – especially trying to push off from the toes at the end of the step
Tight fitting shoes or shoes with high heels can often aggravate symptoms. Certain activities, such as spending long periods walking or standing, may worsen bunion symptoms.
WATCH: What Causes Bunions? (1:48)
Causes of Bunions
Once a bunion has formed, it won’t disappear on its own. In fact, without proper treatment, it often gets worse over time. It’s common for people to blame tight or ill-fitting shoes for causing bunions – but it’s not quite that simple.
While footwear can contribute to bunion symptoms, it’s not the only cause. Many researchers say hereditary factors are to blame.
While you do not directly inherit a bunion, you can inherit certain foot structures that encourage them to develop. The most common conditions and factors that increase the risk of bunion development, include:
Overpronation
Overpronation changes how the big toe experiences stress during walking and running. When the heel tilts toward the inside of the foot, the first metatarsal bone is forced upwards, impacting how the first MTP joint bends. It also causes the small muscles within the foot to pull on the hallux, encouraging it to move toward the other toes.
Arthritis
Osteoarthritis, and systemic arthritis conditions such as rheumatoid arthritis, can encourage bunion development. Arthritis causes inflammation of the joints, damage to joint capsules and lining, and development of bony deformities. If arthritis attacks the first MTP joint, this can result in bunion formation.
Increased mobility in the first metatarsal bone
An increase in movement of the joint, where the first metatarsal bone meets the medial cunieform bone in the middle of the foot, can lead to a lack of stability on this collection of bones, called the first ray.
It is worth noting instability of this first ray at the end of your walking stride. It is when your heel raises, and a majority of your body weight focuses on the first ray. Without adequate stability, loading them can create forces that cause the first metatarsal bone itself to start rotating and deviating outward.
Injuries to the first metatarsophalangeal joint
An existing injury to the first MTP joint can contribute to bunion progression by damaging the joint capsule, encouraging bony overgrowth, and damaging soft tissues that stabilize the bone.
The type of shoes you wear can play a significant role in the development and worsening of bunions. Shoes with tight toe boxes or high heels may encourage symptoms to occur sooner or aggravate existing bunions, especially in people who have a genetic risk of developing them. Keep in mind, bunions progress more rapidly for some people and slower for others; not every case is the same.
Will I develop bunions?
The best predictor of bunion development is looking at family history. You are more at risk if your parents – or close relatives – have bunions. Research has shown some benefit to treating the bunion early on before a more severe deformity appears.
Treatments can include changes to footwear, physiotherapy, manual therapy, custom orthotics, injections to the joint, and surgery. If you see that a bunion is developing, or you have looked at your parent’s feet and know what might be coming, take proactive steps now. A Kintec pedorthist can evaluate your feet and see can be done to help lessen the risk.
References
Dayton P, Kauwe M, Feilmeier M. Is our current paradigm for evaluation and management of the bunion deformity flawed? A discussion of procedure philosophy relative to anatomy. The Journal of Foot & Ankle Surgery 54 102-111, 2015.
Cho B, Park J, Choi S, Soo Hoo N. Is generalized ligamentous laxity a prognostic actor for recurred hallux valgus deformity? Foot and Ankle Surgery 25, 127-131, 2019.
Ferrari J, Higgins JPT, Prior TD. Interventions for treating hallux valgus (abductovalgus) and bunions. Cochrane Database of Systematic Reviews 2004, Issue 1. Art. No.: CD000964. DOI: 10.1002/14651858.CD000964.pub2.
Coughlin M, Jones C. Hallux Valgus: Demographics, etiology, and radiographic assessment. Foot & Ankle International, 2007.
Reina M, Lafuente G, Munuera P. Effect of custom-made foot orthoses in female hallux valgus after one-year follow up. Prosthetics and Orthotics International, 37 (2) 113-119, 2012.
Dayton P, Kauwe M, Feilmeier M. Clarification of the anatomic definition of the bunion deformity. The Journal of Foot and Ankle Surgery, Vol 53 (2), 160-163, 2014.
Doty JF, Alvarez RG, Ervin TB, Heard A, Gilbreath J, Richardson N. Biomechanical evaluation of custom foot orthoses for hallux valgus deformity. The Journal of Foot & Ankle Surgery, 54, 852-855, 2015.
To Kai-Tsun M. Bunion: To treat or not to treat. Editorial in Journal of Orthopaedics, Trauma and Rehabilitation, 19, 2015.
Lowery NJ, Wukich DK. Adolescent hallux valgus: Evaluation and treatment. Operative Techniques in Orthopaedics, Elsevier Inc. doi: 10.1053/j.oto.2009.07.001, 2009.
Isabella
January 15, 2021 at 8:57 pmThank you for providing this wonderful information. Bunions is a bony bump that grows along the side of your big toe. It should be treated early as possible.
Some useful tips that might help you:
1) Avoid wearing heels or shoes that cause discomfort
2) Select wider shoes that can provide more comfort and reduce pain
3) Use Orthotics or foot inserts