Lower Back Pain: A Best Practices Approach
Lower back pain is classified as pain within the lower two quadrants of the back, typically starting from the twelfth rib, down to the pelvis. It can also include the back of the hip – or sacral area. For this reason, sacroiliac pain and lower back pain are often grouped together.

How Common is Lower Back Pain?
It’s estimated up to 80% of people will experience back pain in their life. Globally, and at any point in time, 18% of the population has lower back pain. Over a one-month period, that number is 31%. Lower back pain is found to be more common in women. (Lin et al. 2013)
This chronic health problem forces more people out of the workforce than heart disease, diabetes, hypertension, neoplasm, respiratory disease, and asthma combined. It is also the leading cause of years lived with a disability and the sixth highest cause of global overall disease burden. (Meyer et al. 2017; Schofield et al. 2015)
Lower back pain often requires older workers to retire prematurely. As a result, people with lower back pain retiring earlier have 87% less total wealth than those who are employed full-time.
READ MORE: Managing and Preventing Lower Back Injury
What Contributes to Lower Back Pain?
While lower back pain is common, there is no conclusive data as to what causes it. 80 – 90% of low-back pain is non-specific, meaning clinical diagnostic tests don’t reliably tell why we experience most types of pain.
Researchers speculate that contributing factors include sedentary lifestyles, carrying more weight on our trunk than needed, and not being able to engage stabilizing muscles in the correct way.
Movement & Lower Back Pain
Every movement we make requires stabilization in the back, which is why lower back pain can be so profoundly disabling. When you experience back pain, your first instinct might be to rest and resist moving. However, moving around might help more when it comes to easing back pain.
In fact, research has shown that lower back pain wasn’t as disabling until the introduction of Western Medicine. Historically, Western Medicine relied on diagnostic imaging to determine structural pathology and recommended bed rest and medication for treatment. Studies further suggest that reducing activity without a corresponding reduction in pain can then promote a fear of movement making the pain even more difficult to treat. (Krestiansen et al. 2014; Bergbom at al. 2011; Bergsten et al. 2012)
We now know that the best thing you can do for lower back pain is to incorporate simple – but effective – motions into your daily routine, such as standing and walking. If even simple everyday movements are too painful, or if the pain is not improving noticeably in seven days, we recommend consulting a medical professional.
A physiotherapist or a physician with sports medicine training can perform a more thorough assessment of your back and prescribe a more specific set of movement progressions. If these motions are too difficult for you, there are tools to help you achieve your daily activity goals as prescribed by a professional.
WATCH: 3 Devices To Help Treat Lower Back Pain (2:16)
4 Devices to Help Manage Lower Back Pain
Foot orthotics, back braces, proper footwear, and trekking poles can help you achieve your daily activity goals if you find it difficult to move as much as you need to.
1. Foot Orthotics
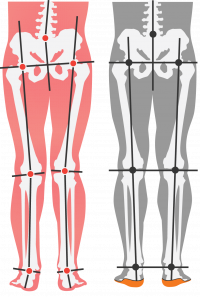
It has been proven that the posture of your feet and ankles can affect hip posture. When the foot and ankle flatten, they can create a motion that causes the hip to roll inward. As your hip rotates inwards, it stretches and activates muscles in the lower back; they have origins in structures in the lower back.
Therefore, it is possible to experience pulling on one side more than the other, especially if one side is flatter than the other. This would create a poor foundation for the lower back structures.
READ MORE: Lower Back Pain and Orthotics
Accepting this information, using orthotics will help reduce how much the foot flattens and reduces how much the hip rotates inward, which will take the strain off these muscles.
A study on shoe orthotics and their role in treating chronic lower back pain, from the Archives of Physical Medicine and Rehabilitation, showed wearing foot orthotics help lower the mean low back pain significantly over the course of 12 months.
2. Back Brace

Many patients find they can move more confidently with less pain when they use a lumbar support brace. In fact, a series of studies have shown that back braces reduce pain while participants walked on a treadmill. (Anders et al., 2016) These studies also showed that lumbar braces helped activate the back’s stabilizing muscles. This suggests these supports would be a good way to complement a patient’s movement goals.
At Kintec, we carry the Bauerfeind Lordoloc, suitable to wear as back support and to stabilize the lumbar spine.
3. Proper Footwear


When choosing footwear to help alleviate back pain, consider a shoe with a stabilizing element and/or a heel pitch.
Stabilizing elements in shoes control the motion of your foot and ankle joints. By reducing motion, particularly pronation, accompanying internal leg rotation, and dropping pelvis there is less strain on the back.
Kintec recommended shoe with stabilizing elements: Mens Asics Kayano 26, Womens Asics Kayano 26
Heel pitch refers to the elevation of your heel over the forefoot. Elevating your heel will allow more range at your ankle when walking, reducing the amount your hip and back have to be active during forward movements.
Kintec recommended shoe with heel pitch: Mens Mizuno Wave Rider 23, Womens Mizuno Wave Rider 23 (12 mm heel drop)
4. Trekking Poles

Also known as Nordic Walking Poles, trekking poles make it easier to work harder. They distribute the effort throughout your body as you use more muscle, burn more calories, and stay more comfortable while walking. Several models of trekking poles are available on the market, all of which suit unique activity goals.
Talk to a Team of Specialists
If your lower back pain hasn’t shown signs of improvement, work with a team of various specialists to manage your symptoms.
Using a multi-disciplinary approach, a pedorthist can help connect you with a team of professionals who can help you manage your back pain. Physiotherapists, sports-medicine trained physicians and physiatrists can be important partners in both building, and evaluating your treatment plan; they can help provide a structured approach and determine where to start you, with regard to exercise and activity management.
Are you experiencing back pain?
Book an appointment with one of our Canadian Certified Pedorthists today for a thorough assessment and personalized treatment plan.
Our new One2One program will provide you with the highest level of safety and personalized service for all of your orthotics, footwear, and bracing needs.

Dr. Sanjay Sharma
July 13, 2020 at 4:08 amThese tips are very helpful, as a doctor I am also a therapist and teach these exercises to my patents. Thanks!
Michael Ryan - Director of R&D
July 22, 2020 at 1:54 pmOur pleasure!